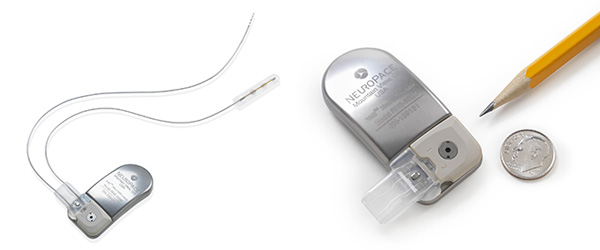
Responsive Neurostimulation (RNS)
Significantly reduces seizures in patients with drug-resistant epilepsy
What is responsive neurostimulation?
If your child has tried two anti-seizure medications, and is still having seizures, they may have drug-resistant epilepsy. According to the Institute of Medicine, about 800,000 Americans experience seizures despite taking anti-seizure medications. In fact, after trying two medications, the chance a third medication will control seizures is less than 5% (Chen, Z. et al. JAMA Neurol. 2018 Mar 1;75(3):279-286).
Seizures result from abnormal electrical discharges in your child’s brain, activity which is very difficult to see. Responsive Neurostimulation (RNS) allows our doctors to see what’s happening in your child’s brain during their normal daily activities. The device collects ongoing information that helps better control your child’s seizures. In clinical studies, the RNS System was shown to significantly reduce seizures with continued improvement over time. Patients also reported better cognitive function, quality of life and mood.
RNS for your child?
The RNS system is used to treat children with partial onset epilepsy who have failed treatment with at least two seizure medications. Our approach is always to determine whether patients are candidates for resection of their seizure focus first. Patients are considered candidates for RNS when they have undergone comprehensive diagnostic testing that has localized one or two seizure foci, but are determined not to be candidates for surgical resection for a particular reason, such as:
- Seizures that originate from more than one area of the brain.
- Seizures that arise from areas of the brain that cannot be resected without causing a deficit.
- Seizures that are difficult to discretely localize.
Additional requirements are:
- 18 years of age or older.
- Frequent and disabling seizures impacting quality of life.
The Placement Procedure
RNS is a breakthrough surgical approach to treating seizures unable to be controlled by medication. The RNS neurostimulator is a battery-powered device placed within a small tray in a child’s skull by a pediatric neurosurgeon. It does not touch the brain, and it rests underneath the scalp, not visible to the child or anyone else. The neurostimulator is connected to two tiny electrodes placed either on the surface of the brain, into the brain or a combination of both. The neurostimulator is programmed by a pediatric neurologist to detect a child’s seizures, even during periods of sleep. When a seizure or seizure-like activity is detected, within milliseconds, the device sends brief pulses to the brain to stop, shorten or possibly even prevent the seizure altogether. The pulses normalize brainwaves, often before a child can feel seizure symptoms.
Thee electrodes also continuously record and collect brainwave data, seizure activity and patient progress. This information gives us a better understanding of our patients’ seizures, allowing us to design the best course of treatment in a real-time, ongoing basis.
The procedure typically requires only a 1 to 2 night hospital stay, and the battery in the neurostimulator is estimated to last about eight years.
How effective is RNS?
In clinical trials, more than half of the patients treated with RNS had 50% or fewer seizures compared to their pre-surgical baseline. Perhaps more importantly, most patients reported significant improvement in their quality of life with RNS. It is important to keep in mind seizure reduction from RNS is not immediate. It may take several months to notice improvement and it will possibly take years to achieve the optimal results.
Follow-up to the RNS Procedure
Parents who choose RNS for their child play a key role in their care. Families are given a remote monitor, which is essentially a laptop computer, where they must download information stored on their child’s neurostimulator on a daily basis. This process takes just a few minutes a day. Once a week, they are asked to upload the data stored on their child’s remote monitor to a secure website database where their child’s doctors can review it. Patients’ parents are given a wand and are asked to swipe the wand over their child’s neurostimulator when they have a seizure. This action marks that particular event as important and the device stores the child’s brain activity recorded during that time so the doctor can take a closer look at it.